What is personalised medicine?
Shot of a doctor showing a patient some information on a digital tablet

Personalised medicine looks at a person’s individual genes, environment and lifestyle to guide decisions about their healthcare and the prevention, diagnosis and treatment of specific conditions.
- Personalised medicine moves away from a ‘one-size-fits-all’ approach when preventing, diagnosing and treating diseases. Instead, it considers a person’s unique genomics, environment and lifestyle to make decisions about their healthcare.
- It’s a relatively new field with the potential to improve outcomes for patients, by matching a person to the right healthcare for them at the right time.
What is personalised medicine?
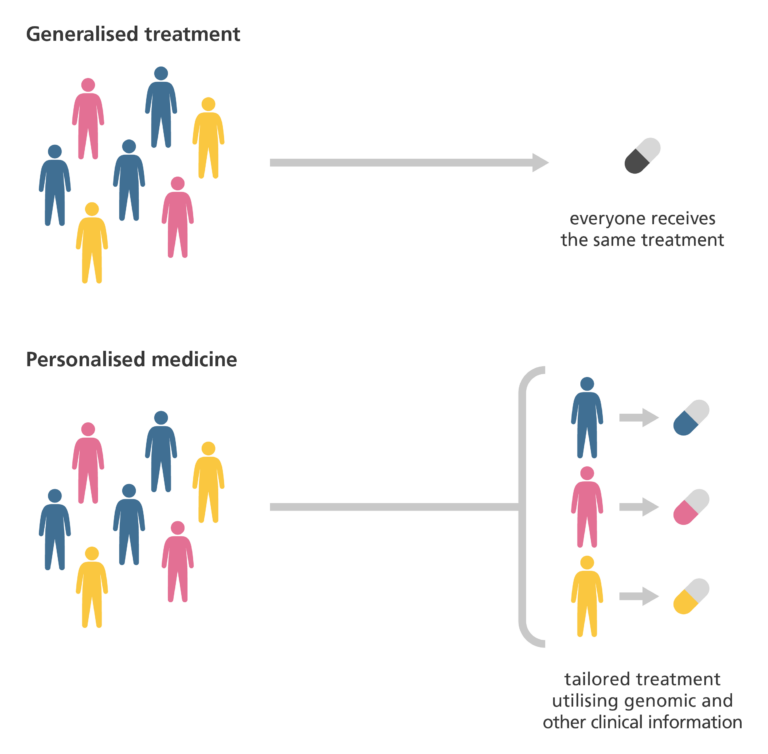
- Historically, medicines have been designed and tested to work for the ‘average’ person. However, when we consider the ways that we’re all different, the averages used in designing medicine don’t work for everyone - and are usually biased in terms of sex and ethnicity.
- If a group of people all took the same medicine for the same illness, they would likely respond differently. Many would see their health improve. Some would experience side effects. Some might not gain any benefits from the medicine.
- That’s because our health is determined by a unique combination of genes, lifestyle and environments. Thanks to advances in genomics and technology, medical research can now take these differences into account.
- By scouring healthcare data and looking for patterns, scientists can predict outcomes for different combinations of characteristics. For some healthcare, doctors can now use this information to guide how they should treat their patients most effectively.
- This is sometimes called precision medicine.
What are the advantages of personalised medicine?
- In 2000, the first human genome was sequenced – and it cost £2 billion.
- Today, costs have dramatically reduced, making it easier and more affordable to sequence a person’s genome and understand how their genetics influences their health. We can also sequence at specific regions of the genome for conditions where the genetics are well known, such as cystic fibrosis or haemophilia.
- We’re already using this information for some healthcare decisions, such as matching people with cancer to the right treatment for them.
- As technology continues to advance, personalised medicine could become a routine part of healthcare – potentially benefiting individuals, the wider population, healthcare systems and medical research. For example:
- People may have underlying conditions detected more effectively using better diagnostic tests.
- Doctors may be able to use genomic tests to work out which medicine is the best option for each patient, with the lowest risk of side effects. This could also save time and cost for healthcare systems.
- Scientists may be able to develop more effective medicines that target specific genomic characteristics and to design more efficient clinical trials.